Restoring Proteostasis May Boost T Cell Function and Open a New Route for Immunotherapy
30 April 2026
Key Takeaways
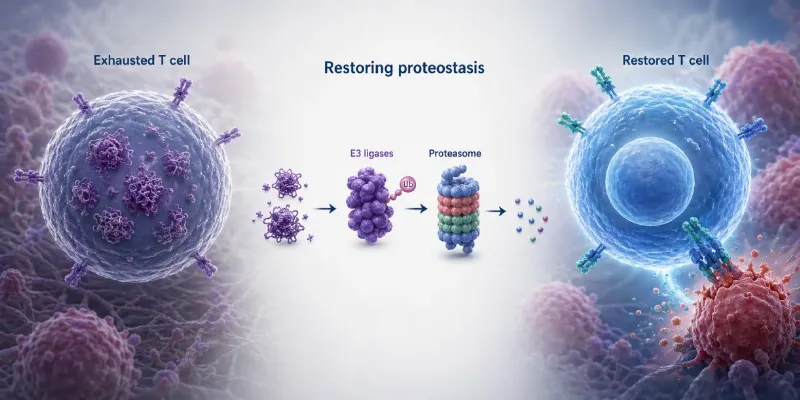
- A new Cell study suggests that T cell exhaustion in tumors is driven in part by failed proteostasis, causing damaged and misfolded proteins to accumulate inside tumor-infiltrating lymphocytes.
- Restoring three E3 ubiquitin ligases, NEURL3, RNF149, and WSB1, cleared this buildup and improved T cell function in preclinical models.
- The findings highlight a potential new strategy for enhancing cancer immunotherapy.
T cells are among the immune system’s most powerful weapons against cancer. Yet inside tumors, even these highly specialized cells can lose momentum. After repeated exposure to cancer antigens, tumor-infiltrating lymphocytes often enter a dysfunctional state known as T cell exhaustion, becoming less capable of killing malignant cells. A new study published in Cell suggests that one reason for this decline may lie in a surprisingly basic cellular process: protein recycling.
The research, led by Professor Ananda Goldrath’s laboratory at the University of California San Diego, identifies a breakdown in proteostasis, the system that helps cells fold, maintain, transport, and clear proteins. In exhausted T cells, this network appears to falter, allowing damaged and misfolded proteins to accumulate. The findings open a potential therapeutic path: restoring the cell’s internal protein quality-control machinery to help T cells regain antitumor function.
“We found that exhausted T cells’ recycling programs are falling apart, leading to damaged and misfolded proteins that pile up with nowhere to go,” said Nicole Scharping, a postdoctoral fellow in Goldrath’s lab and lead author of the study.
Why proteostasis matters in exhausted T cells
T cell exhaustion is a central obstacle in cancer immunotherapy. Tumor-infiltrating lymphocytes, or TILs, may initially attack cancer cells but progressively differentiate into terminally exhausted states that limit durable tumor control. In contrast, tissue-resident memory T cells, known as TRM cells, can remain functional in healthy tissues for years, and tumors enriched with TRM-like TILs have been associated with better prognosis.
The new study compared different T cell populations using proteomic and transcriptomic profiling. Researchers found that TRM cells and progenitor-exhausted T cells, which retain more therapeutic potential, shared expression of genes linked to proteostasis. Terminally exhausted T cells, by contrast, showed a clear loss of proteostasis, including accumulation of unfolded proteins.
Importantly, the problem was not simply a defective proteasome, the cellular machinery that degrades proteins. The researchers found evidence of unfolded protein buildup despite functional proteasome activity. This suggested a failure upstream, in the system that tags proteins for degradation.
That tagging system depends in part on E3 ubiquitin ligases, enzymes that help label damaged or unwanted proteins so they can be removed. Mass spectrometry, performed with collaborators at UC San Diego and the La Jolla Institute for Immunology, helped identify three ligases, NEURL3, RNF149, and WSB1, as key candidates involved in restoring this recycling function.
Scharping described the approach as a “tag and sort” fix, comparing the ligases to labelers in a recycling facility.
“In exhausted T cells, many of these enzymes get switched off, and recycling grinds to a halt,” said Scharping. “When we restored specific E3 ligases, the buildup cleared, and the T cells regained their function and worked better at clearing tumors.”
A biological bridge between cancer immunity and protein-aggregate disease
The study also points to a broader biological theme. Cells that fail to manage damaged or misfolded proteins can develop toxic aggregates, a phenomenon better known in neurodegenerative diseases. The researchers suggest that exhausted T cells may share certain cellular stress features with conditions such as Parkinson’s and Alzheimer’s disease.
“We think this loss of proteostasis resembles what occurs in neurons in other protein aggregate diseases such as Parkinson’s and Alzheimer’s,” said Ananda Goldrath, a professor in the Department of Molecular Biology. “Rescuing these cells from exhaustion could improve the ability of T cells to respond to both chronic infection as well as tumors.”
This comparison does not mean T cell exhaustion is the same as neurodegeneration. Rather, it highlights a shared vulnerability: when cellular quality-control systems fail, function declines. In cancer, that decline may blunt the immune response at precisely the moment when durable activity is needed.
Implications for cancer immunotherapy
In preclinical models, enforced expression of NEURL3, RNF149, and WSB1 helped preserve stem-like TCF1-positive T cell populations, improved T cell function in tumors and chronic infection, and reduced the accumulation of unfolded proteins in TILs. Deficiency in these ligases impaired tumor-infiltrating lymphocytes and altered T cell differentiation during acute infection.
The findings are especially relevant for cell-based immunotherapies, where T cell fitness is critical. If engineered or expanded T cells can be modified to maintain proteostasis, they may remain functional longer within the hostile tumor microenvironment. The study suggests that reinforcing E3 ligase activity could potentially improve the potency and durability of cancer cell therapies.
“We uncovered one of the mechanisms by which T cells lose their ability to fight cancer and now we have a target that we can use to design interventions to improve responses to immunotherapy as well as prevent chronic infection,” said Goldrath.
Still, the work remains preclinical. The experiments were conducted in mice, and translating these findings into human cancer therapy will require further validation. Researchers will need to determine whether the same proteostasis defects occur across human tumor types, whether these ligases can be safely manipulated, and how such interventions might integrate with existing checkpoint inhibitors, adoptive T cell therapies, or other immunotherapy platforms.




Comments
No Comments Yet!