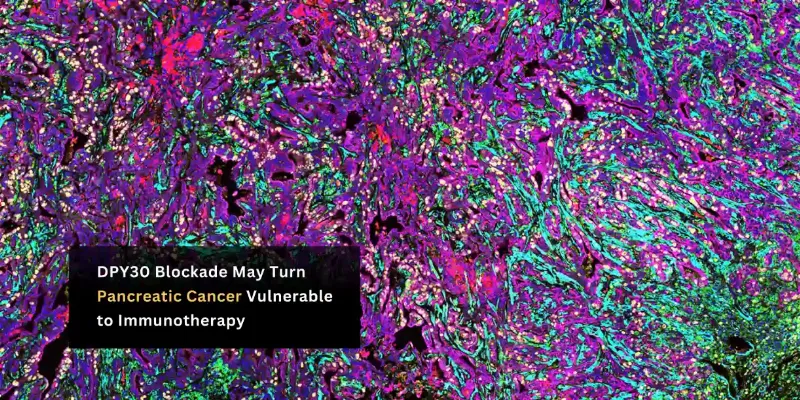
MD Anderson Study Identifies DPY30 as Therapeutic Target in Pancreatic Cancer
11 April 2026
Key Takeaways
- DPY30 has emerged as a potential therapeutic target in pancreatic cancer, where immunotherapy has shown limited benefit.
- Loss of DPY30 destabilized replication forks, triggered inflammatory signaling, and increased T-cell infiltration, making tumors more visible to the immune system.
- In patient samples, high DPY30 expression was associated with poorer prognosis and weaker response to immunotherapy.
- The findings suggest DPY30 could serve both as a predictive biomarker and as part of future combination strategies designed to make pancreatic tumors more responsive to immunotherapy.
Immune checkpoint inhibitors have transformed care in several cancers, but pancreatic tumors usually remain immunologically “cold,” with little T-cell infiltration and limited responsiveness. A new study from researchers at The University of Texas MD Anderson Cancer Center points to a possible way to change that, by targeting an epigenetic factor called DPY30.
Published in Cancer Research, the study was led by Francesca Citron, Pharm.D., Ph.D., instructor of Genomic Medicine, and identifies DPY30 as a regulator that helps pancreatic cancer cells withstand DNA replication stress, a hallmark of aggressive tumors. When that protection is lost, replication forks become unstable, inflammatory signaling rises, immune cells infiltrate the tumor, and the cancer becomes more sensitive to immune checkpoint blockade.
A different role for a familiar epigenetic protein
DPY30 is a component of the WRAD/COMPASS histone methyltransferase complex, which is generally known for regulating gene expression through chromatin modification. But this study argues that DPY30 has a more specialized function in pancreatic cancer. Rather than broadly controlling transcription like other WRAD components, DPY30 appears to act directly at stressed DNA replication forks.
There, it promotes H3K4me3 deposition, helping preserve fork stability and maintain genomic integrity under replication stress. That distinction matters. The authors describe DPY30 not simply as another chromatin regulator, but as a replication stress-specific epigenetic modifier, one that allows tumor cells to withstand ongoing DNA damage without broadly rewiring transcription.
Turning instability into immune visibility
The most intriguing finding is what happens when DPY30 is lost. According to the abstract, DPY30 deficiency destabilized stalled replication forks, leading to fork degradation, chromosomal instability, and inflammation, yet without suppressing cancer cell proliferation. That combination is biologically important. It suggests that removing DPY30 does not merely poison the tumor, it changes how the tumor is perceived by the immune system.
In experimental models, this loss promoted T-cell infiltration and improved tumor responsiveness to immune checkpoint blockade. In effect, interfering with DPY30 helped convert pancreatic tumors from immune-excluded lesions into tumors more capable of being recognized and attacked.
That mechanistic link between replication stress and immunoediting is the central advance of the study. It suggests that epigenetic control at replication forks may shape not only tumor survival, but also immune escape.
A potential biomarker for patient selection
The translational angle is equally notable. In patient samples, higher DPY30 expression was associated with more aggressive disease features, poorer prognosis, and inferior response to immunotherapy. That raises the possibility that DPY30 could serve as a predictive biomarker, helping identify which patients are less likely to benefit from checkpoint inhibition alone, and which might be candidates for combination approaches.
“Understanding this new function of DPY30 as an epigenetic switch suppressing DNA replication stress in cancer cells can have a tremendous impact on future therapeutic strategies for pancreatic cancer patients, especially in combination with immunotherapy,” Francesca Citron said. “We are encouraged by the potential to investigate this protein both as a predictive biomarker and as a therapeutic target to enhance immunotherapy response for patients with pancreatic cancer, who currently have limited effective treatment options.”
The study does not yet establish a ready-to-use therapy. Still, the concept is compelling: instead of trying only to stimulate immunity from the outside, researchers may be able to reprogram pancreatic tumors from within by exploiting a specific vulnerability in how they manage replication stress.



Comments
No Comments Yet!