PSMA PET/CT May Transform Prostate Cancer Diagnosis and Reduce Biopsies by 50%
13 March 2026
New findings from the phase III PRIMARY2 trial presented at EAU26 suggest that PSMA PET/CT imaging after inconclusive or reassuring MRI can safely reduce prostate biopsies by about 50 percent without missing clinically significant cancers. In a study of 660 high-risk individuals, the scan accurately distinguished aggressive tumors from indolent disease and helped guide targeted biopsies, potentially improving diagnostic precision while reducing overdiagnosis.
The results, presented at the European Association of Urology Congress (EAU26), may advance molecular imaging and reshape the diagnostic pathway for prostate cancer.
Rethinking the Diagnostic Pathway
Prostate cancer evaluation typically begins with magnetic resonance imaging (MRI) to identify suspicious lesions within the prostate. When MRI findings are inconclusive or moderately suspicious, patients are often advised to undergo biopsy. Although biopsy remains the diagnostic gold standard, it is an invasive procedure associated with discomfort, anxiety, and potential complications.
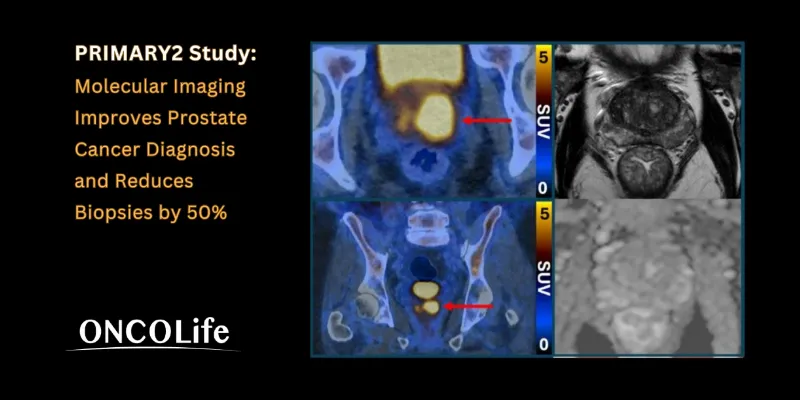
The PRIMARY2 study examined whether molecular imaging could refine this diagnostic pathway. Researchers evaluated the role of prostate-specific membrane antigen (PSMA) PET/CT scanning, an imaging technique that highlights prostate cancer cells by using a radiotracer molecule that selectively binds to PSMA proteins expressed on tumor cells. Once bound, these cells appear as bright signals on the scan, enabling clinicians to detect biologically active disease.
The PRIMARY2 Trial
The trial enrolled 660 individuals at increased risk of prostate cancer, including those with a strong family history, whose MRI results were normal or inconclusive. Participants were randomly assigned to undergo either standard biopsy or PSMA PET/CT imaging.
The results indicate that PSMA PET/CT could effectively identify patients who either did not have cancer or whose tumors were biologically indolent and unlikely to cause harm. In these cases, biopsy could safely be avoided. Conversely, patients with positive PSMA PET/CT findings proceeded to targeted biopsy directed toward suspicious areas identified by the scan.
This strategy reduced the number of biopsies by approximately half without missing clinically significant cancers. In patients who did require biopsy, the imaging results improved procedural precision by guiding sampling toward suspicious regions, potentially reducing complications and improving diagnostic accuracy.
Dr James Buteau, a nuclear medicine physician at Peter MacCallum Cancer Centre who presented the findings, emphasized the clinical implications of the technology: PSMA PET/CT scanning makes prostate cancer cells light up in a remarkable way, particularly in more aggressive cancers. It’s rare to see such strong imaging that could be so powerful in the clinic. Incorporating this testing into clinical care could help to address the major challenge of prostate cancer overdiagnosis, which leads to at best unnecessary and at worst harmful treatment for cancers that would never cause any harm.”
Addressing the Challenge of Overdiagnosis
Overdiagnosis remains a persistent challenge in prostate cancer screening and diagnosis. Detecting low-risk tumors that may never progress can lead to overtreatment, exposing patients to unnecessary therapies and associated side effects.
A Complementary Imaging Strategy
The investigators describe the approach as a complementary diagnostic strategy that enhances existing imaging methods. By integrating PSMA PET/CT after MRI, clinicians may gain a more precise understanding of tumor biology before recommending invasive procedures.
Professor Louise Emmett, Director of Theranostics and Nuclear Medicine at St Vincent's Hospital and co-lead investigator of the study, explained: “Getting told you have a risk of prostate cancer is a huge cause of anxiety and concern. Our findings show that PSMA PET/CT after MRI offers a 'belt and braces' approach that can determine which people have a clinically significant cancer, and which people are at low risk and don’t need a biopsy or further testing. PRIMARY2 is the largest of a series of studies undertaken by this group, exploring whether PSMA PET/CT scanning could improve prostate cancer diagnosis and reduce unnecessary biopsies for patients.”
Participants in the PRIMARY2 trial will continue to be followed for two years to evaluate longer-term outcomes. If confirmed, these findings could support a shift toward more precise and less invasive diagnostic strategies in prostate cancer care, reducing unnecessary procedures while preserving accurate detection of clinically significant disease.
PRIMARY2 Study, PSMA PET/CT, Prostate Cancer, Diagnosis, Biopsies, overdiagnosis


Comments
No Comments Yet!